Temporomandibular disorder, or TMD, describes a range of issues arising from in and around the temporomandibular joint (TMJ). These involve: night-time grinding or clenching; tooth wear and cracks in teeth; clicking or pain when opening and closing the lower jaw; pain resulting from long periods of mouth opening; or limited capacity for mouth opening. The causes of these symptoms usually have many factors involved.
So where do we start? Firstly, your general dentist will assess your symptoms and possible causes of TMD, then will tailor your treatment accordingly.
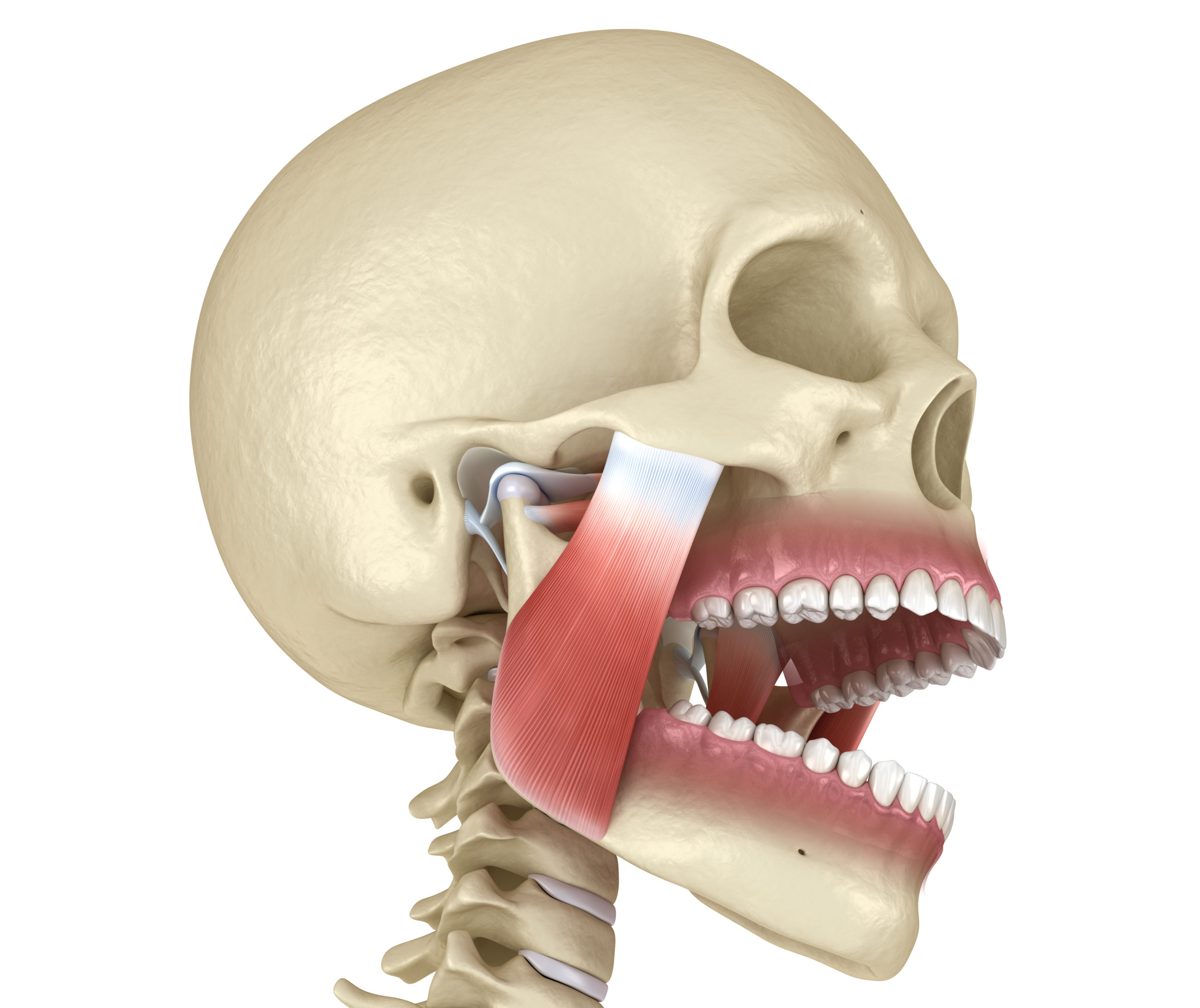
Causes of TMD
Congestive sleep apnoea: occurs as a result of your tongue rolling back in your mouth at night, blocking your airways. Grinding and clenching may occur as an attempt to wake yourself up at night. Specialised splints or C-PAP machines can be useful in treating this condition.
Crooked teeth have been occasionally associated with TMD, though usually when there are more significant bite problems. Teeth straightening, at times with jaw repositioning surgery, may help to reset your bite into a more harmonious position.
Anxiety, stress, and personality quirks may just lead some people to grind without any other clearly defined cause.
What are the treatment options?
Splints
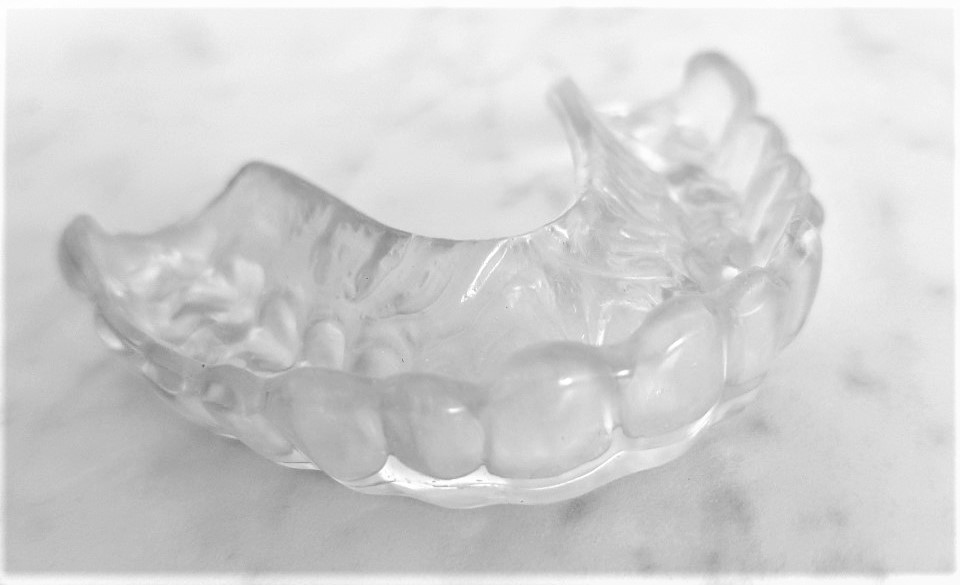
If sleep apnoea and bite discrepancies don’t seem to play a large role we usually start with a splint. This is a clear plastic mouthguard you wear on your top teeth at night. These are specially fitted for your teeth so they don’t fall out easily and provide an even bite with a free range of movement. These will not stop your grinding or clenching, but it will help to reduce it and ease forces. The plastic material acts as a buffer between your teeth and protects them from wear and cracks. The splint can look bulky at first, but after a couple of weeks most people adapt fairly well. For our splints, we use a hard firm material on the outside and a gel layer on the inside fitting surface. These are generally reported as far more comfortable than the standard plain hard splint design.
Muscle Relaxant Injectables
Muscle relaxant injectables provide an alternative to those who find a splint still too bulky. These can be injected into the overworked, enlarged chewing muscles. The masseters, bands of thick muscle at the back of your jaws, are usually injected first and reviewed 4-6 weeks later. The muscles will lose some strength so that they will naturally release when clenched, easing tightness. The temporalis, a band over the temple and stretching laterally across the skull, may also require injecting. The injectables typically last 4-6 months and can be seen to slim the jawline giving a nice aesthetic side effect.

Other treatments
Physiotherapy can also be used as an adjunct to the prior treatment methods. This will focus on improving range of motion and decreasing tension. If your TMD is a little more complicated you may require a more specialised splint, anti-inflammatory or anti-anxiety medications. If there are physiological changes to the joints then surgery may be required. Arthritis or other changes can occur when TMD has been present for a long time without adequate intervention. These can be difficult to treat and may only provide a small improvement, therefore early management of TMD is critical.



Hey very nice blog!